|
12/27/2022 1 Comment Eyes hurt when i move them
There are two types of headaches: tension and cluster. The pressure behind your eye could come down to a simple headache or even a more serious migraine. Soon, the pressure behind your eyes will disappear on its own. Let your eyes rest away from the screen, book, or windshield. The best treatment for eye strain is to take a break. Some of the other symptoms of this condition are blurry vision, dry eyes, and pressure in your socket. Staring at a screen for most of the day, reading small print, or driving for a long period of time can cause eye strain. It happens when your eyes get tired from consistent use. Eye StrainĪlthough eye strain isn’t a medical condition, it’s a very common cause of feeling pressure behind your eye. You can find over-the-counter treatment for your eye pressure at a local pharmacy. These mild illnesses and conditions are very common. 8 Common Causes for Feeling Pressure Behind Your Eye Find out what it could be, and what you should do when you feel pressure behind your eye. Most times, the cause of pain or pressure behind your eyes comes down to a mild illness that’s easy to treat.īut, if it’s persistent, it may be a sign of a graver problem. It’s also worrying to imagine what this symptom means. 2020 92:589–594.Feeling pressure behind your eye is very uncomfortable. Evaluation of coronavirus in tears and conjunctival secretions of patients with SARS-CoV-2 infection. 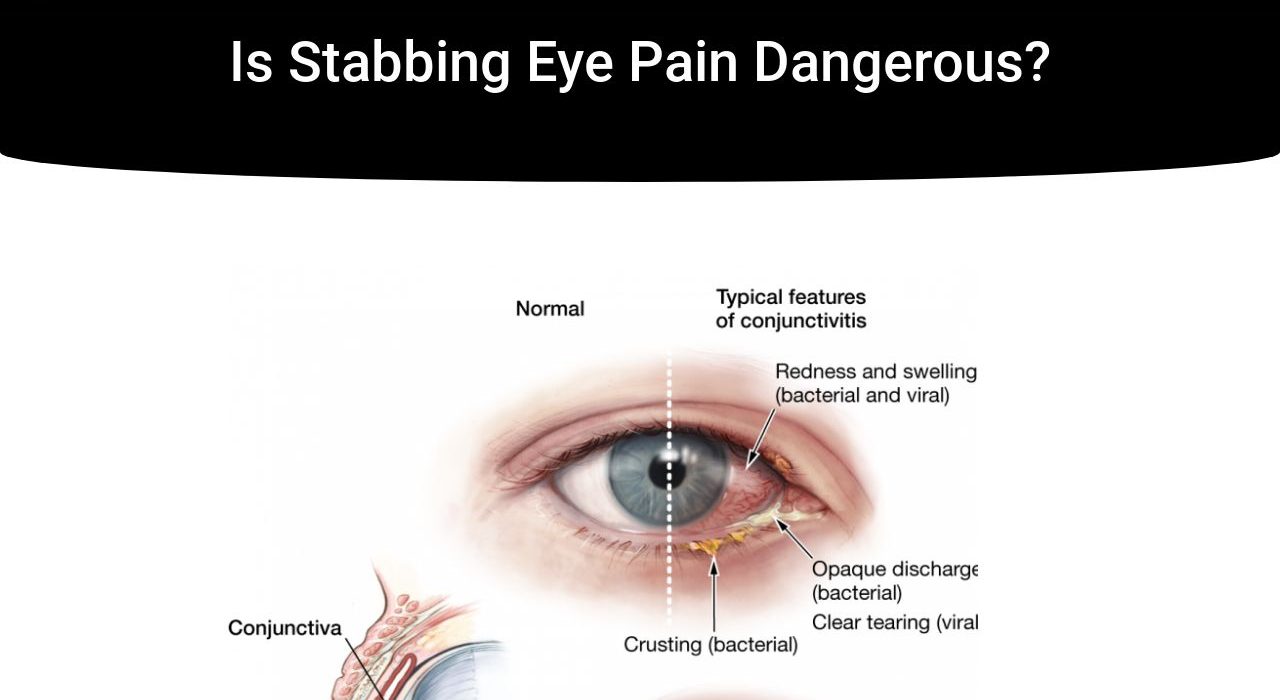
Clinical characteristics of coronavirus disease 2019 in China. Guan W, Ni Z, Hu Y, Liang W, Ou C, He J, Liu L, Shan H, Lei C, Hui D, Du B, Li L, Zeng G, Yuen K, Chen R, Tang C, Wang T, Chen P, Xiang J, Li S, Wang J, Liang Z, Peng Y, Wei L, Liu Y, Hu Y, Peng P, Wang J, Liu J, Chen Z, Li G, Zheng Z, Qiu S, Luo J, Ye C, Zhu S, Zhong N. The most common causes of eye pain at 2 tertiary ophthalmology and neurology clinics. Accessed June 28, 2021.īowen RC, Koeppel JN, Christensen CD, Snow KB, Ma J, Katz BJ, Krauss HR, Landau K, Warner JEA, Crum AV, Straumann D, Digre KB. 
WHO Statement Regarding Cluster of Pneumonia Cases in Wuhan, China. Finally, investigation into the COVID-19-associated headache phenotype of those with a history of migraine may have broader implications, adding to a more general understanding of migraine pathology.Ĭopyright © 2022 by North American Neuro-Ophthalmology Society. Early identification of headache class could assist in predicting the clinical course of disease. In addition, investigation of headaches associated with COVID-19 demonstrated 4 distinct phenotypes that follow third edition of the International Classification of Headache Disorders categories: headaches associated with personal protective equipment, migraine, tension-type headaches, and COVID-19-specific headache. Furthermore, eye pain during COVID-19 may provide evidence of hypersensitivity-type reactions, neurovirulence, and incitement of either novel or subclinical autoimmune processes. These presentations add to a more complete picture of SARS-CoV-2 viral transmission and mechanism of host infection. 
Four distinct COVID-19-related headache phenotypes were identified and discussed.Įye pain in the setting of COVID-19 presents as conjunctivitis, episcleritis, scleritis, or optic neuritis. The literature search led to a focused review of COVID-19 associated with conjunctivitis, episcleritis, scleritis, optic neuritis, and myelin oligodendrocyte glycoprotein-associated optic neuritis. The primary search was conducted in June 2021. Reports of ocular manifestations of vision loss in the absence of eye pain were excluded. Where SARS-CoV-2 research was deficient, pathology of other known viruses was considered. Case reports, literature reviews, and meta-analyses were all included. Literature was mined from the PubMed database using the key terms: "eye pain," "conjunctivitis," "episcleritis," "optic neuritis," "migraine," and "headache" in conjunction with "COVID-19" and "SARS-CoV-2." With the exception of general background pathology, articles that predated 2006 were excluded. This literature review aims to describe presentations of eye pain and headache in relation to COVID-19, with an emphasis on how these disorders help us to understand the pathophysiology of COVID-19. Although its respiratory effects can be deadly and debilitating, it can lead to other systemic disorders, such as those causing eye pain and headache. Severe acute respiratory syndrome-coronavirus-2 (SARS-CoV-2), which causes Coronavirus Disease 2019 (COVID-19), emerged in December 2019 and became a devastating pandemic. 
1 Comment
Joyce
1/23/2023 03:28:28 pm
Very well done! Your insights have guided me for sure. I want to share a clinic that specializes in eye healthcare. "Eye Connection". https://www.eyeconnection.com.au They have quality optometrists and offer the widest range of glasses. Thanks again!
Reply
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
